Rehab insurance verification: 3 Easy Steps 2025
Introduction: Why Verifying Your Insurance is the First Step to Recovery
When facing addiction, the cost of treatment can be a major hurdle. That’s where rehab insurance verification comes in. It’s the process of checking your health insurance benefits to see what addiction treatment services your plan covers, helping you understand your financial responsibility and removing barriers to getting the help you need.
Here’s a quick overview of what rehab insurance verification means for you:
- What it is: Checking your health insurance benefits to see what addiction treatment services your plan covers.
- Why it’s done: To understand your financial responsibility and remove financial barriers to treatment.
- How it works: Typically done by the rehab center’s admissions team, or you can call your insurance provider directly.
Many people delay getting help due to money worries. However, recent laws like the Affordable Care Act (ACA) mandate that most health insurance plans cover addiction treatment like any other medical illness. This means your insurance might cover more than you think.
Understanding your insurance benefits for rehab can feel confusing. You might worry about privacy or what information is needed. But getting this clear early on provides peace of mind and allows you to focus on recovery, not unexpected bills. This guide will walk you through each step simply and clearly.
Understanding Your Coverage: What Your Insurance Plan Means for Rehab
Understanding your health insurance plan is the clearest path to covering your rehab costs. It’s your map to seeing what services are covered, what you might pay out-of-pocket, and which treatment centers are the best fit. Getting to know your policy is key to open uping its full potential.
Fortunately, landmark laws have greatly expanded insurance coverage for mental health and substance use disorders. The Affordable Care Act (ACA) mandates that most health plans cover “Essential Health Benefits,” which include mental health and substance use disorder services. This has made treatment accessible to millions more Americans. You can learn more on the official HHS website: Affordable Care Act (ACA).
Additionally, the Mental Health Parity and Addiction Equity Act (MHPAEA) of 2008 requires large group health plans to provide mental health and substance use disorder benefits that are on par with medical and surgical benefits. This ensures fair coverage and makes it easier to access life-changing treatment. For more details, visit the SAMHSA website: Mental Health Parity and Addiction Equity Act (MHPAEA).
When looking for a rehab facility, you’ll hear terms like “in-network” and “out-of-network.” This distinction is important because it affects your costs. “In-network” providers have pre-negotiated rates with your insurance company, which means lower out-of-pocket expenses for you, with your plan often covering 60% to 90% of the cost. “Out-of-network” providers don’t have this agreement, so your costs will likely be higher, and your plan may cover a much smaller percentage, if anything.

Commonly Covered Services and Key Terms
Thanks to these laws, most insurance plans cover a wide range of addiction treatment services. Your plan might cover Detoxification (Detox), medically supervised care to manage withdrawal symptoms. It often covers Inpatient or Residential Treatment, where you live at the facility for intensive, 24/7 care. For those who need intense support but can live at home, Partial Hospitalization Programs (PHP) offer structured day treatment. A step down, Intensive Outpatient Programs (IOP) provide significant therapy with more flexibility. Less intensive, Outpatient Treatment is ideal for ongoing support. Many plans also cover Medication-Assisted Treatment (MAT), which combines medication with counseling.
As you review your policy, you’ll see key terms that describe your costs:
Your Deductible is the amount you must pay for covered services before your insurance plan starts to pay. For example, with a $3,000 deductible, you pay the first $3,000 of covered care.
A Copayment (Copay) is a fixed amount you pay for a covered service after meeting your deductible, like a $25 fee for a doctor’s visit.
Coinsurance is your share of the cost for a covered service, calculated as a percentage after your deductible is met. If a service is $100 and your coinsurance is 20%, you pay $20.
Finally, the Out-of-Pocket Maximum is your financial safety net. It’s the absolute most you’ll pay for covered services in a plan year. Once you reach this limit, your plan pays 100% of covered benefits for the rest of the year.
Understanding these terms is crucial for anticipating your financial commitment and ensuring a smooth rehab insurance verification process.
How Your Plan Type Affects Coverage
The type of health insurance plan you have affects your access to rehab and your out-of-pocket costs. Here’s a quick look at common plan types:
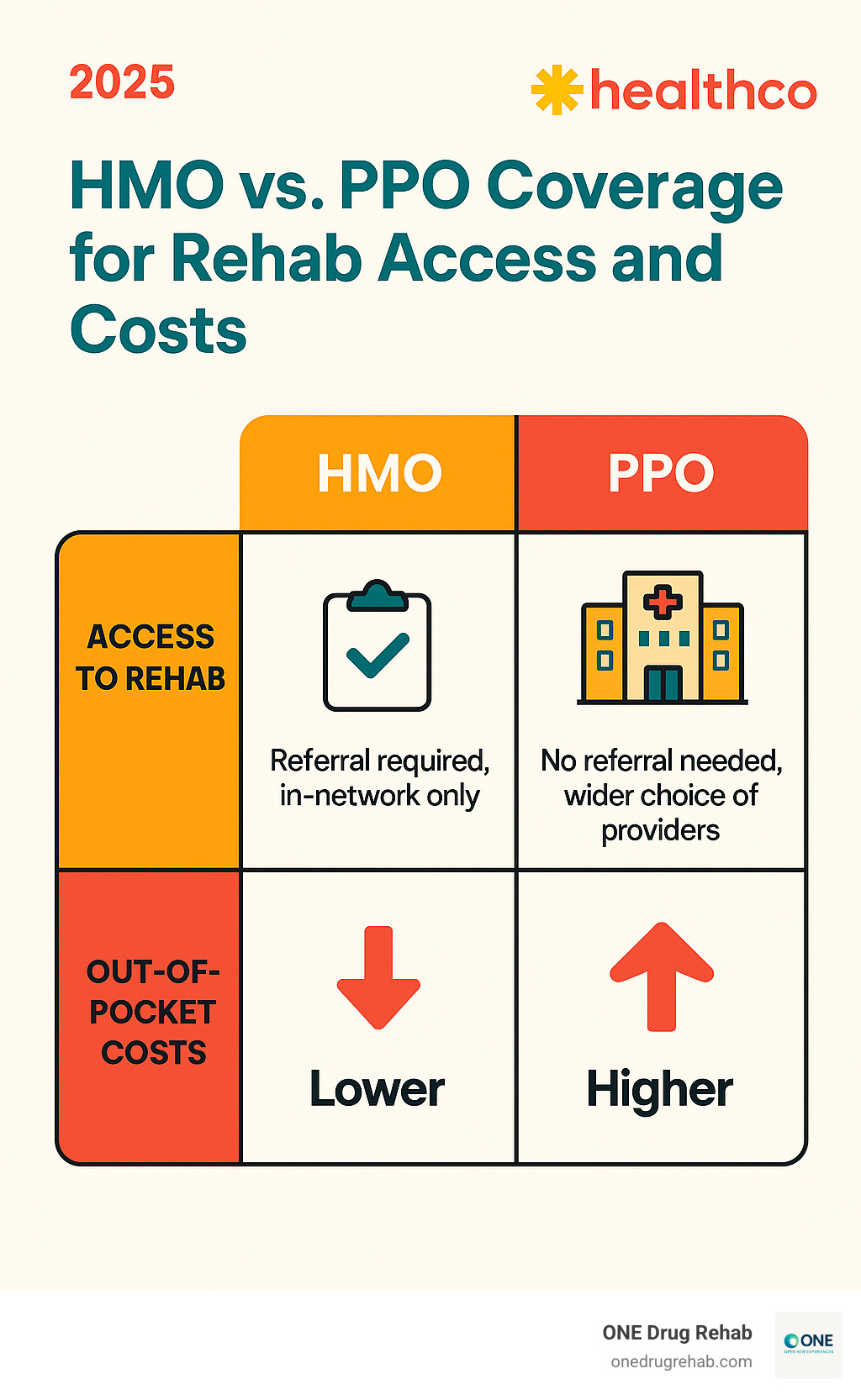
- Health Maintenance Organization (HMO): HMOs often have lower premiums but require you to use a primary care provider (PCP) for referrals to in-network specialists and facilities. Care outside the network is generally not covered, except in emergencies.
- Preferred Provider Organization (PPO): PPOs offer more flexibility, as you typically don’t need a referral to see a specialist. You can use out-of-network providers, but your costs will be higher. This gives you a wider choice of rehab centers.
- Exclusive Provider Organization (EPO): EPOs are a hybrid. You don’t usually need a referral, but like HMOs, they won’t cover care outside their network, except for emergencies.
- Point of Service (POS): POS plans combine HMO and PPO features. You choose a PCP but have the option to go out-of-network for care, though you’ll pay more for that extra flexibility.
Your plan type directly impacts your freedom in choosing a rehab facility and how much you’ll pay. Always review your policy or speak with your insurance provider to understand these details for a smoother rehab insurance verification.
The Step-by-Step Guide to Rehab Insurance Verification
Now that you understand the insurance jargon, let’s walk through the actual rehab insurance verification process. This crucial step confirms your coverage and helps you move forward. While it might seem daunting, it’s a straightforward process used by thousands of people annually, and your information is always handled with the utmost confidentiality.

Step 1: Preparing for Your Rehab Insurance Verification
Preparation is key to a smooth rehab insurance verification. Before you begin, gather the necessary information to make the process quicker and more accurate. You’ll typically need:
- Patient Information: Full legal name, date of birth, and contact information.
- Policyholder Information: If the patient is not the primary policyholder, you’ll need the full legal name, date of birth, and contact details of the insured individual.
- Insurance Card Details: The name of your insurance carrier, your member ID number, group number (if applicable), and the insurance company’s phone number (often on the back of the card).
- Potential Rehab Facility Details (if known): Having a facility’s name and location is helpful for checking in-network status.
Having these details ready ensures a precise verification of your benefits.
Step 2: How to Complete the Rehab Insurance Verification Process
Once your information is ready, there are a few ways to complete the rehab insurance verification:
- Contacting Your Insurance Company Directly: Call the number on your insurance card (often a separate line for behavioral health). Ask about your coverage, specific covered services, costs (deductible, copay, coinsurance), and any pre-authorization requirements for rehab.
- Using a Rehab Center’s Verification Service: Most reputable rehab facilities offer a complimentary insurance verification service. Their admissions team are experts at navigating insurance. You provide your information, and they contact your provider on your behalf, explaining your benefits as they apply to their programs. This is often the easiest route.
- Using an Online Verification Tool: Many treatment providers offer online forms to submit your insurance information. These tools can often provide instant results, confirming if your provider covers addiction-related treatments. This is a quick way to get an initial understanding of your benefits.
No matter the method, the goal is to get a clear picture of your coverage before committing to treatment.
Step 3: What Happens After Verification is Complete?
Once your rehab insurance verification is done, you’ll receive a detailed breakdown of your benefits, often called a Verification of Benefits (VOB). This will outline:
- Covered Services: Which types of treatment (detox, inpatient, etc.) are covered.
- Coverage Levels: The percentage your insurance will pay for in-network vs. out-of-network care.
- Deductible and Out-of-Pocket Status: How much of your deductible you’ve met and your out-of-pocket maximum status.
- Pre-authorization Requirements: Some treatments require prior approval from your insurance company. This is a critical step to ensure coverage, and the rehab center’s admissions team typically handles it for you.
After the VOB, an admissions navigator from the rehab center will contact you. They’ll explain your benefits, discuss potential costs, and help you make an informed decision.
It’s important to know that the rehab insurance verification process is confidential. Your information is protected by federal laws like HIPAA (Health Insurance Portability and Accountability Act) and 42 CFR Part 2. HIPAA governs the use of your health information, while 42 CFR Part 2 specifically protects the privacy of individuals seeking substance use treatment. This means your insurance provider and employer will not be notified without your consent. You can learn more about these protections here: HIPAA and 42 CFR Part 2.
Navigating Challenges and Advocating for Your Benefits
Sometimes, challenges can arise during the rehab insurance verification process. Insurance denials or limitations can occur, but don’t despair. There are strategies to help you advocate for the coverage you deserve.

Advocating for Your Coverage
If your insurance coverage for rehab is limited or denied, it’s not the end of the road. Here’s how you can advocate for your benefits:
- Understand the Reason for Denial: The insurance company must provide a reason for denial, such as “lack of medical necessity.” Understanding this is the first step to an appeal.
- Gather Documentation: Collect all relevant medical records and recommendations from healthcare professionals to support the medical necessity of the treatment.
- Appeal the Decision: You have the right to appeal an insurance denial. Start with an internal appeal, and if that fails, you can pursue an external review through an independent third party.
- Document Everything: Keep detailed records of all communications with your insurance provider, including dates, times, names, and reference numbers.
- Use Specialists: Many rehab centers have dedicated insurance specialists or advocates who can help you steer the appeals process. You can also find third-party advocacy services that specialize in helping patients secure their benefits.
- Leverage Legislative Acts: Remind your insurance company of the Mental Health Parity and Addiction Equity Act (MHPAEA) and the Affordable Care Act (ACA), which mandate coverage for addiction treatment.
How does insurance coverage work for multiple rehab stays? This varies by policy, treatment history, and medical necessity. Insurers may scrutinize repeated stays more closely, but demonstrating a continued commitment to recovery and providing clear medical justification can help. Some plans assign a care manager to help coordinate and authorize care. Always verify benefits for each stay.
What If Insurance Isn’t Enough? Exploring Alternative Payment Options
Even after your rehab insurance verification, you might find a gap between your coverage and the full cost of treatment. Or perhaps you don’t have insurance. Don’t let financial worries stop you from getting help. There are many ways to make rehab affordable.
Don’t hesitate to ask rehab facilities about payment options. Many understand financial problems and offer flexible payment plans, allowing you to pay the balance in manageable installments. This can relieve significant pressure.
Some centers also use a sliding-scale fee system, where the cost of treatment adjusts based on your income. This is designed to make quality care accessible to more people.
Rehab scholarships and grants are also available from non-profits and government programs. These are funds you don’t have to pay back. You can explore options through resources like SAMHSA (Substance Abuse and Mental Health Services Administration) or by asking the admissions team at a rehab facility.
Another option is crowdfunding on websites like GoFundMe, where you can ask your community for financial support. It can be powerful to see people rally around you.
Personal loans or credit cards can provide immediate funding if other options aren’t available, but be sure to weigh the costs of interest carefully.
Lastly, look into state-funded programs. Many states offer publicly funded rehab for those with lower incomes or no insurance. These may have waiting lists but provide crucial, low-cost or free care.
At ONE Drug Rehab, we believe financial worries shouldn’t block the path to recovery. We’re here to help you find resources. You can explore general options for applying for rehab on our platform: Apply for Rehab. Plus, we have information on understanding payment options to help you plan: Rehab Payment & Checkout.
Frequently Asked Questions about Rehab Insurance and Costs
It’s natural to have more questions about the financial side of addiction treatment. Let’s tackle some of the most common concerns so you can feel more prepared.
Are rehab costs tax deductible?
Yes, in some cases, rehab costs can be tax deductible. The IRS allows you to deduct medical expenses, including addiction treatment, that exceed 7.5% of your adjusted gross income (AGI). For example, if your AGI is $75,000, you could deduct medical expenses over $5,625. Be sure to keep detailed records of all treatment-related costs, including program fees and travel. Since tax laws are complex, it’s best to consult a qualified tax professional to understand your specific situation.
Does attending rehab affect life insurance policies?
Yes, attending rehab can affect life insurance policies. Insurers view a history of substance abuse as a risk factor, which may lead to higher premiums or a waiting period for coverage. However, this shouldn’t deter you from seeking help. Demonstrating long-term stability and sobriety can significantly improve your chances of getting favorable rates. Insurers look for proof of sustained recovery, and some specialized insurers have more experience working with individuals with a history of addiction. The long-term health benefits of sobriety far outweigh potential life insurance complications.
Is the rehab insurance verification process confidential?
Yes, the rehab insurance verification process is highly confidential. Strong federal laws protect your privacy, so you can seek help without fear of your information being shared inappropriately. Two key laws provide this protection:
- HIPAA (Health Insurance Portability and Accountability Act): This law sets strict rules on how your health information can be used and disclosed, generally requiring your consent.
- 42 CFR Part 2: This is an even stricter federal regulation that safeguards the privacy of records for individuals seeking drug or alcohol treatment.
You may also wonder, will your employer find out if you go to rehab? Generally, no. You are not required to disclose your specific medical condition to your employer. You can use protections like the Family and Medical Leave Act (FMLA) for job-protected leave without revealing private details. Professional addiction treatment will not appear on a standard background check. These legal protections allow you to focus on recovery with peace of mind.
Conclusion: Take the Next Step with Confidence
Taking the first step towards recovery is a brave decision that can change your life. We know that treatment costs can feel overwhelming, which is why understanding your rehab insurance verification is so important. It lifts a huge weight off your shoulders, letting you focus on healing, not bills.
In this guide, we’ve explained why verifying your insurance is vital, how laws like the ACA and MHPAEA protect you, and what key insurance terms mean. We’ve provided a step-by-step verification guide, tips for advocacy, and alternative payment options.
This knowledge is power. You are informed about your rights and the strong privacy protections from HIPAA and 42 CFR Part 2. There’s no need for confusion or fear to hold you back. You have the information to move forward.
At ONEDrugRehab.com, we’re here to help you find your way. We offer general information and help you explore your choices. Think of us as a friendly guide, pointing you toward the information you need to make the best decisions for you.
So, take a deep breath. You’ve got this. Take that next step with confidence.




