Why Behavioral Therapy Matters in Addiction Recovery
Behavioral therapy addiction treatment has become one of the most effective tools for helping people overcome substance use disorders. If you’re trying to understand how this approach works, here’s what you need to know:
Quick Answer: What is Behavioral Therapy for Addiction?
- What it is: A practical, short-term form of psychotherapy that helps people change the thoughts and behaviors driving their substance use
- How it works: Identifies triggers, challenges negative thinking patterns, and builds healthier coping skills
- Treatment length: Typically 12-20 sessions, though some see results in as few as 4-6 sessions
- What it treats: Alcohol, opioids, cocaine, methamphetamine, and other substance use disorders
- Insurance: Usually covered by insurance, Medicare, and Medicaid under mental health parity laws
The journey to recovery from addiction can feel overwhelming. You might be wondering which treatment approach will actually work, or if therapy can really make a difference when medications seem more straightforward.
Here’s the truth: decades of research show that behavioral therapy—especially Cognitive Behavioral Therapy (CBT)—is highly effective for treating addiction. It’s not about endless talk therapy or digging through childhood memories. Instead, it’s a practical, action-focused approach that gives you specific tools to manage cravings, avoid relapse, and build a life without substances.
Most people with alcohol or drug use disorders struggle with underlying mental health issues too. Behavioral therapy addresses both the addiction and the thoughts and feelings that fuel it. It teaches you to recognize the patterns keeping you stuck and replace them with healthier responses.
The best part? Research shows that combining behavioral therapy with medication produces even stronger results than either approach alone. You’re not choosing between therapy and medication—you’re using the most powerful tools available.
Handy behavioral therapy addiction terms:
Understanding Cognitive Behavioral Therapy (CBT) for Addiction
Let’s start with the basics. What exactly is Cognitive Behavioral Therapy (CBT)? At its heart, CBT is a practical, short-term form of psychotherapy designed to help people develop skills and strategies for becoming and staying healthy. Unlike some other therapies that dig deeply into past issues, CBT focuses on the “here-and-now” – the problems that arise in our day-to-day lives. It’s a structured, time-limited, problem-focused, and goal-oriented approach that aims to change negative thought patterns to change behaviors.
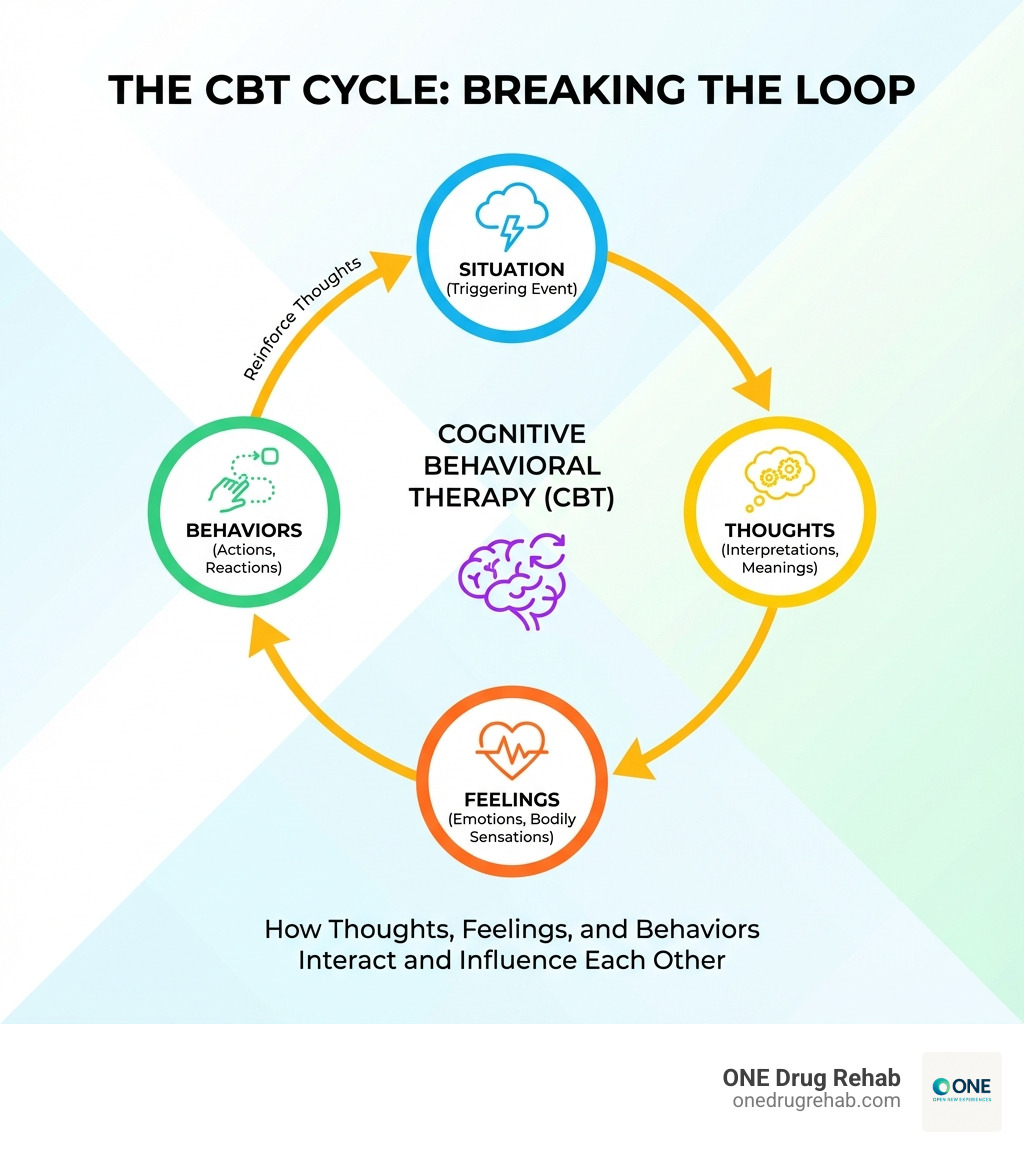
The core of CBT lies in its emphasis on the relationship between our thoughts, feelings, and behaviors. We all have ways of making sense of the world around us, and these perceptions profoundly affect how we feel and act. CBT helps us examine these perceptions and understand their impact.
The CBT model is built on a two-way relationship between our thoughts (cognitions) and our behaviors. Each influences the other. For instance, if we think, “I can’t cope with stress without a drink,” that thought can lead to feelings of anxiety, which then drives the behavior of drinking, reinforcing the initial thought. This cycle can be tough to break, but CBT provides the tools to do just that.
For a deeper dive into how CBT works, you can watch this insightful video: In this video, Dr. Zindel Segal, a CBT expert, discusses how CBT works.
A key part of CBT involves identifying negative thought patterns. We learn to monitor and record our thoughts during upsetting situations, which helps us see how our thinking contributes to emotional problems like depression and anxiety. Once identified, CBT teaches us to question and change these thoughts, recognize distortions in our thinking, and view thoughts as mere ideas rather than undeniable facts. This allows us to step back and consider situations from different viewpoints, opening the door to healthier responses.
Developing healthy coping skills is another cornerstone of CBT. This means learning practical strategies to manage daily life, including those challenging moments that might trigger substance use.
The Core Idea: Connecting Thoughts and Behaviors
The fundamental principle behind CBT is that psychological disorders, including addiction, are based, in part, on inaccurate ways of thinking and learned patterns of negative behavior. It’s not just about what we do, but why we do it, and the thoughts that lead us there.
We all develop learned patterns of behavior, some of which can become maladaptive, especially when influenced by negative and positive reinforcements related to substance use. These patterns interfere with our ability to achieve our goals and live a meaningful life. CBT helps us understand these patterns and develop better ways of coping, relieving symptoms and creating positive changes.
The two-way relationship between thoughts and behaviors is central. Our thoughts influence our feelings and actions, and our actions can, in turn, reinforce our thoughts. This creates a powerful cycle that can either perpetuate addiction or facilitate recovery.
CBT categorizes cognition into three levels:
- Conscious thoughts: These are the thoughts we are actively aware of and can verbalize.
- Automatic thoughts: These are quick, often subconscious thoughts that pop into our heads in response to situations. They can be highly influential in driving our feelings and behaviors.
- Schemas: These are deeply held core beliefs or assumptions about ourselves, others, and the world. They act as filters through which we interpret experiences and can underlie many automatic thoughts.
By understanding these levels, we can begin to challenge and change them. Behavioral change techniques are then employed to break negative cycles. These include self-monitoring (tracking our thoughts and behaviors), activity scheduling (planning positive activities), and exposure and response prevention (facing fears or triggers in a controlled way to reduce their power).
How CBT Works for Substance Use Disorders
When it comes to behavioral therapy addiction treatment, CBT is particularly effective. It directly addresses the cognitive and environmental factors that contribute to substance use.
Here’s how it works in the context of addiction:
- Identifying Triggers: CBT helps us pinpoint the specific thoughts, emotions, and external situations that trigger cravings or the urge to use substances. This could be anything from stress at work to feeling lonely, or even seeing a certain place or person.
- Correcting Maladaptive Thinking: Many individuals with substance use disorders hold beliefs that justify their use (e.g., “I need alcohol to relax,” or “drugs help me escape my problems”). CBT challenges these misguided thinking patterns, helping us re-evaluate them in light of reality. We learn to identify distortions in our thinking and see these thoughts as ideas, not facts.
- Enhancing Motivation for Change: Through collaborative discussions and exercises, CBT helps us strengthen our resolve to change and commit to a life free from substances. It empowers us to believe in our ability to manage difficult situations without resorting to old habits.
- Developing Healthy Coping Skills: This is crucial for long-term recovery. CBT teaches us a range of alternative coping skills to deal with stress, cravings, and difficult emotions. Examples include setting realistic goals, building social supports (like attending 12-Step meetings), learning effective communication skills, engaging in various forms of exercise, and practicing relaxation techniques.
- Relapse Prevention: CBT models are highly beneficial for relapse prevention. By targeting cognitive and environmental triggers and promoting alternative coping skills, we learn to anticipate high-risk situations and develop strategies to steer them without relapsing. This proactive approach helps us build resilience and maintain abstinence.
Core Principles and Applications of Behavioral Therapy for Addiction

The core principles of behavioral therapy addiction treatment are rooted in empowering individuals to take control of their thoughts and actions. It’s about giving us the tools to understand why we use substances and how to choose healthier responses. This proactive approach is a significant reason for its success.
A major focus of CBT in addiction treatment is relapse prevention. It’s not enough to stop using; we also need to learn how to stay stopped. CBT provides training in behavioral self-control skills to help us achieve and maintain abstinence or harm reduction. This time-limited, multisession intervention targets the cognitive, affective, and environmental risks that lead to substance use.
Integral to this process is psychoeducation, where we learn about addiction as a disease, its triggers, and the mechanics of relapse. This knowledge empowers us to approach our recovery with a clear understanding. Coupled with this is skills training, where we actively practice new ways of thinking and behaving.
To hear more about the broader role of therapy in addiction, consider listening to this perspective: The role of therapy in addiction treatment.
The Primary Goals of CBT in Addiction Treatment
When we engage in CBT for addiction, we’re working towards several key goals:
- Developing Awareness: We aim to become acutely aware of our misguided thinking patterns that contribute to our problems. This self-awareness is the first step toward change.
- Re-evaluating Thinking: Once aware, we learn to critically examine and re-evaluate these thoughts in light of reality. We challenge irrational beliefs and replace them with more balanced and realistic perspectives.
- Understanding Motivation: We strive to understand the underlying motivations behind our own behaviors and those of others, especially concerning substance use. This helps us gain insight and empathy.
- Problem-Solving Techniques: CBT equips us with realistic problem-solving techniques. Instead of resorting to substances when faced with challenges, we learn constructive ways to address them.
- Building Confidence: As we successfully apply new skills and strategies, our confidence in our ability to manage stressful situations grows. This empowerment is vital for sustained recovery.
- Calming the Mind and Body: Many individuals use substances to self-medicate anxiety or distress. CBT teaches us techniques to calm our minds and bodies naturally, enabling us to face our fears instead of avoiding them.
What Types of Addictions Can CBT Treat?
CBT is a versatile and evidence-based therapy that has been successfully adapted to treat a wide range of mental health issues and substance use disorders. Its effectiveness stems from its core principles, which can be applied across different addictive behaviors.
Here are some of the types of addictions and related conditions that behavioral therapy addiction (CBT) can help treat:
- Alcohol Use Disorder (AUD): CBT is a first-line behavioral approach for AUD, helping individuals manage cravings, identify triggers, and develop coping skills for abstinence.
- Opioid Use Disorder: CBT is effective in both standalone and combined treatment strategies for opioid addiction, focusing on relapse prevention and managing withdrawal symptoms.
- Cocaine Dependence: CBT has demonstrated efficacy in treating cocaine dependence, often integrated with other modalities.
- Methamphetamine Use Disorder: CBT helps individuals with methamphetamine addiction by addressing thought patterns and behavioral responses associated with stimulant use.
- Cannabis Use Disorder: Similar to other SUDs, CBT helps individuals identify triggers and develop strategies to reduce or cease cannabis use.
- Other Substance Use Disorders: The principles of CBT can be applied to various other substance addictions, as it focuses on universal cognitive and behavioral mechanisms.
- Co-occurring Disorders: A significant strength of CBT is its ability to treat co-occurring mental health conditions that often accompany addiction. These include:
- Depression: CBT is particularly effective in addressing negative thought patterns associated with depression.
- Anxiety Disorders: This includes Generalized Anxiety Disorder (GAD), Panic Disorder, and specific phobias. CBT teaches skills to manage anxiety and avoid using substances as a coping mechanism.
- Post-Traumatic Stress Disorder (PTSD): CBT can help individuals process traumatic memories and reduce the need to self-medicate with substances.
- Eating Disorders: CBT helps address distorted body image and unhealthy eating patterns.
- Obsessive-Compulsive Disorder (OCD): CBT techniques can manage compulsive behaviors and intrusive thoughts.
- Bipolar Disorder, Schizophrenia, and Psychosis: While often used in conjunction with medication, CBT can help manage symptoms and improve coping in these complex conditions.
The CBT Experience: What to Expect from Treatment

Starting on behavioral therapy addiction treatment can feel like a big step, and it’s natural to wonder what the experience will be like. Rest assured, CBT is a highly individualized treatment, meaning it will be custom to your specific needs and challenges. It’s also a deeply collaborative process between you and your therapist, working together as a team towards your recovery goals.
CBT sessions are typically structured, which can be a comforting framework, especially when dealing with the chaos that addiction often brings. The focus is always on practical, problem-solving strategies.
A Look Inside a Typical CBT Session for Behavioral Therapy Addiction
When you step into a CBT session for addiction, you can expect a proactive and engaging environment. This isn’t just about talking; it’s about doing.
- Therapist-Client Collaboration: From the very first session, you and your therapist will work hand-in-hand. This shared therapeutic relationship is fundamental. Your therapist guides you, but you are an active participant in your own healing.
- Setting Goals: Together, you’ll define clear, achievable goals for your recovery. These goals are practical and present-focused, such as reducing cravings, avoiding specific triggers, or improving communication with loved ones.
- Functional Analysis of Substance Use: You’ll spend time analyzing your substance use patterns. This involves identifying the situations, thoughts, and feelings that lead to using, as well as the consequences of that use. Understanding these patterns is crucial for breaking them.
- Skills Training Exercises: Your therapist will teach you specific strategies and skills to manage your addiction. This might include techniques for identifying and challenging negative thoughts, learning relaxation methods, or developing assertiveness skills to refuse substances.
- Role-Playing Scenarios: To prepare you for real-world challenges, you might engage in role-playing. This allows you to practice new coping strategies in a safe environment, rehearsing how to handle high-risk situations or difficult conversations.
- Homework Assignments: Yes, there’s homework! CBT is about applying what you learn. Between sessions, you’ll be given “homework” assignments, such as monitoring your thoughts, practicing new skills, or engaging in planned positive activities. This helps consolidate improvement and empowers you to manage your recovery independently.
Treatment Duration and Insurance Coverage for Behavioral Therapy Addiction
One of the benefits of CBT is that it’s often a short-term therapy. For issues like anxiety and depression, treatment usually involves 12 to 20 sessions. However, the length of treatment can vary considerably depending on the severity and complexity of your individual problems. Some people might see significant improvement in as few as four to six sessions, while others may require more than 20 sessions to achieve their goals. Weekly sessions typically last for two to three months, making it a relatively efficient approach.
The good news is that behavioral therapy addiction treatment, including CBT, is typically covered by insurance. The Affordable Care Act (ACA) mandates that health insurance companies must cover mental health and substance use disorders on par with coverage for medical or surgical procedures. This means that your insurance plan should provide coverage for CBT if it’s deemed medically necessary.
Furthermore, Medicaid is the largest payer for mental health services in the United States, and the ACA expanded Medicaid benefits to millions of Americans who previously didn’t qualify. All Marketplace plans also cover both mental health and substance use disorder treatments as “essential health benefits.” While coverage details can vary by individual plan and provider, it’s worth checking with your insurance company to understand your specific benefits.
Maximizing Success: Integrating CBT and Finding a Provider
When we talk about maximizing success in addiction recovery, it’s clear that behavioral therapy addiction treatment, particularly CBT, plays a pivotal role. It’s an evidence-based treatment that equips us with practical skills for daily life, fostering a profound sense of empowerment. We learn to steer the complexities of recovery with newfound confidence and resilience.
The Benefits of CBT Compared to Other Approaches
CBT stands out for several compelling reasons when compared to other therapies or no therapy at all:
- Short-Term Format: As a practical, short-term form of psychotherapy, CBT often yields meaningful results in a relatively brief period, typically 12-20 sessions, compared to therapies that might span years.
- Effective Relapse Prevention: CBT is highly effective in relapse prevention, specifically targeting triggers and teaching alternative coping mechanisms, making it a robust tool for maintaining long-term sobriety.
- Learning Practical Skills: We gain concrete, actionable skills to manage our thoughts, emotions, and behaviors in real-time, empowering us to handle life’s challenges without resorting to substances.
- Reduced Emotional Problems: By identifying and challenging distorted thinking, CBT helps reduce emotional problems like anxiety and depression, which are often intertwined with addiction.
- Increased Confidence: Successfully applying CBT techniques builds self-efficacy and confidence in our ability to manage stressful situations and maintain recovery.
- Proactive and Collaborative: The proactive, shared therapeutic relationship encourages active participation and responsibility in our recovery journey, fostering a sense of ownership over our progress.
While CBT is incredibly powerful on its own, it’s important to note that it doesn’t always perform better than other evidence-based behavioral therapies when combined with pharmacotherapy. The key takeaway is that an evidence-based behavioral therapy, like CBT, is crucial.
Integrating CBT with Pharmacotherapy
For many individuals battling addiction, the most effective path to recovery involves a comprehensive treatment plan that combines behavioral therapy addiction with medication-assisted treatment (MAT). This integrated approach is increasingly recognized as a best practice in addiction care.
Combined behavioral and pharmacological interventions have shown significant advantages. For example, meta-analytic evidence strongly supports the efficacy of CBT when integrated with pharmacotherapy. In fact, studies show that effect sizes (indicating treatment effectiveness) were roughly five times higher when CBT was combined with medication than when CBT was delivered as a standalone intervention. This means that while CBT is effective on its own, it becomes even more potent when paired with appropriate medications.
A systematic review and meta-analysis on this very topic concluded that combined CBT and pharmacotherapy was associated with increased benefit compared with usual care and pharmacotherapy. This highlights that for optimal outcomes, best practices in addiction treatment should include pharmacotherapy alongside CBT or another evidence-based therapy, rather than relying solely on usual clinical management or nonspecific counseling services. You can explore more about this research here: Meta-analytic evidence on CBT efficacy.
How to Find a Qualified CBT Therapist
Finding the right therapist is a crucial step in your recovery journey. Here’s how we can go about finding a qualified CBT provider for behavioral therapy addiction treatment:
- Start with Your Insurance Provider: The first step is often to check with your health insurance company. They can provide a list of in-network providers who specialize in CBT and addiction treatment. The Affordable Care Act mandates coverage for mental health and substance use disorders.
- Use Online Directories: Many reputable online directories list licensed therapists by specialty, location, and insurance accepted. Look for therapists who specifically mention experience with substance use disorders and CBT.
- Check Professional Organizations: Organizations like the Association for Behavioral and Cognitive Therapies (ABCT) or the American Psychological Association (APA) often have search tools or directories of qualified professionals.
- Ask for Referrals: Your primary care doctor, another mental health professional, or even trusted friends and family might be able to provide recommendations.
- Look for Medicaid and Medicare Providers: If you’re covered by Medicare or Medicaid, you can find providers who accept these plans. The U.S. Department of Health and Human Services provides resources to help you locate suitable professionals: Find a provider who accepts Medicaid and Medicare.
- Interview Potential Therapists: Don’t hesitate to schedule initial consultations. Ask about their experience treating addiction, their approach to CBT, their typical treatment duration, and what a session would look like. This helps ensure a good fit.
Conclusion: A Practical Path to Lasting Recovery
In conclusion, behavioral therapy addiction treatment, particularly Cognitive Behavioral Therapy (CBT), offers a practical, evidence-based pathway to lasting recovery. We’ve seen how CBT empowers individuals by teaching them to identify and challenge unhelpful thought patterns, develop robust coping skills, and actively prevent relapse. It’s a collaborative journey that focuses on the present, equipping us with tangible tools to manage triggers and build a life free from substance dependence.
The integration of CBT with pharmacotherapy further strengthens treatment outcomes, making a comprehensive, individualized approach the gold standard for addiction care. By understanding how CBT works, what to expect, and how to find a qualified provider, we can take significant steps toward taking control of our thoughts and behaviors.
If you or a loved one are seeking support and ready to explore behavioral therapy options for addiction, we’re here to help. Our directory offers resources to connect you with facilities that provide effective, evidence-based treatment.
Find a treatment center in our directory




