The Reality of Benzodiazepine Dependence and Safe Withdrawal
Benzo withdrawal treatment is a medically supervised process for safely stopping benzodiazepines. It involves gradual dose reduction, symptom management, and support. This is critical because abruptly quitting benzos can cause life-threatening complications like seizures, especially since around 40% of long-term users (6+ months) develop severe withdrawal.
Quick Overview: What You Need to Know
- Primary Approach: Slow, medically supervised tapering over weeks or months.
- Duration: Acute symptoms last 5-28 days; protracted symptoms can persist for months in 10-25% of users.
- Where to Get Help: Medical detox, inpatient rehab, or specialized outpatient care.
- Key Risk: Never quit “cold turkey” due to the risk of seizures and psychosis.
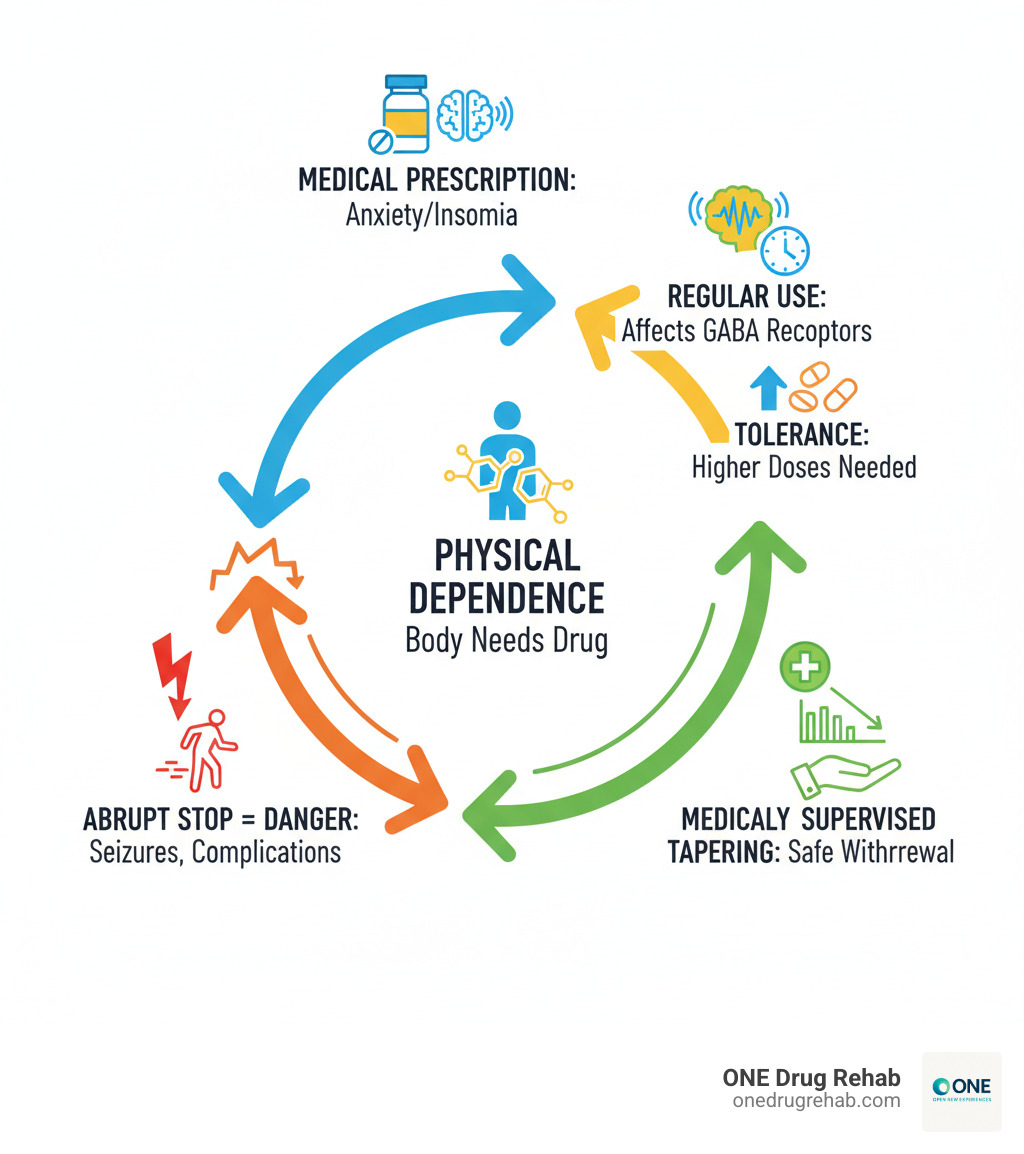
Benzodiazepines—like Xanax, Valium, and Klonopin—are prescribed for anxiety, insomnia, and seizures. They improve the brain’s calming neurotransmitter, GABA. While effective short-term, prolonged use leads to physical dependence as the brain adapts to the drug. When you stop, withdrawal symptoms emerge.
Benzodiazepine withdrawal is medically dangerous, making professional treatment essential. With prescriptions on the rise, more people face this challenge. The good news is that with proper medical supervision and a comprehensive plan, safe withdrawal and full recovery are possible.
This guide will cover what withdrawal involves, why medical supervision is vital, and the treatment options available.
Understanding Benzodiazepine Withdrawal: Symptoms and Timeline
When you stop taking benzodiazepines after developing dependence, your central nervous system goes into shock. Without the drug, a cascade of symptoms emerges, ranging from uncomfortable to dangerous. This is why benzo withdrawal treatment in professional Detox Centers is crucial for managing this process safely.

Primary Symptoms of Benzodiazepine Withdrawal
Withdrawal symptoms affect your mind, body, and perception of reality.
-
Psychological Symptoms: Often, the original anxiety or panic issues return with greater intensity (rebound anxiety). Other common symptoms include panic attacks, irritability, severe insomnia, depression, brain fog, and in severe cases, suicidal thoughts. These are signs of your brain rebalancing.
-
Physical Symptoms: These add another layer of distress. Expect tremors, sweating, muscle pain and stiffness, relentless headaches, nausea, dizziness, and heart palpitations.
-
Perceptual Distortions: Some people experience hypersensitivity, where light seems too bright, sounds are painfully loud, and touch can feel uncomfortable. Others report feeling detached from their body (depersonalization) or reality (derealization). These effects are temporary.
-
Severe Symptoms: These are medical emergencies that require immediate professional care. They include grand mal seizures, which can be life-threatening, and psychosis, which involves hallucinations and delusions. These risks are why you should never quit on your own.
The Typical Withdrawal Timeline
The withdrawal timeline varies based on the benzodiazepine’s half-life—how long it stays in your system.
- Short-acting benzos like alprazolam (Xanax) cause withdrawal to start quickly, within 1-2 hours, peaking in 24-72 hours.
- Long-acting benzos like diazepam (Valium) have a delayed onset, with symptoms appearing 2-7 days after stopping, but they may last longer.
Withdrawal generally occurs in two phases:
-
The Acute Phase: This is the initial, most intense period. Symptoms are at their peak and can be dangerous. It typically lasts 5 to 28 days, though it can be longer for long-acting benzos (2-8 weeks).
-
Protracted Withdrawal Syndrome (PAWS): Affecting 10% to 25% of chronic users, PAWS involves symptoms that continue or fluctuate for months or even years. These symptoms—like lingering anxiety, insomnia, and fatigue—are usually less intense but can be frustrating. Proper benzo withdrawal treatment helps manage both phases successfully.
Key Factors and Risks of Benzodiazepine Discontinuation
Two people on the same benzo dose can have vastly different withdrawal experiences. Benzo withdrawal treatment must be personalized to account for the many factors influencing your body’s response. This complexity is why medical supervision is essential for safety.

Factors Influencing Withdrawal Severity
Your withdrawal experience depends on a unique combination of factors:
- Duration of Use: Dependence can develop in as little as 3-6 weeks. The longer the use, the more the brain adapts, often leading to a more challenging withdrawal.
- Daily Dosage: Higher doses create stronger physical dependence and increase the risk of severe symptoms.
- Type of Benzodiazepine: Short-acting benzos (e.g., Xanax) often trigger more abrupt, intense symptoms, while long-acting ones (e.g., Valium) may allow for a smoother, though longer, withdrawal.
- Method of Discontinuation: Gradual tapering under medical supervision is safe. Abruptly stopping (“cold turkey”) is a medical emergency.
- Co-occurring Disorders: Co-existing mental health or substance use issues can intensify withdrawal symptoms. Integrated Co-occurring Disorder Treatment is vital for addressing all conditions simultaneously.
- Individual Physiology: Age, liver function, and metabolism all affect how your body processes the drug and influence the tapering schedule.
The Dangers of Abruptly Quitting Benzodiazepines
Stopping benzodiazepines suddenly is not just uncomfortable—it is potentially life-threatening. When you quit “cold turkey,” your central nervous system goes into overdrive, which can be catastrophic.
- Grand Mal Seizures: This is the most severe risk. An estimated 20-30% of people in unsupervised withdrawal from sedatives experience seizures, which can be fatal.
- Delirium and Hallucinations: Severe confusion, disorientation, and seeing or hearing things that aren’t there are signs of a medical emergency.
- Psychosis: A complete loss of touch with reality, including paranoid delusions, is a possible and dangerous complication.
- Suicidal Thoughts: The combination of intense anxiety, depression, and physical pain can feel unbearable, leading to a significant risk of suicide.
The VA guidelines on tapering confirm that abrupt discontinuation after even one month of daily use can be severe. If you take benzodiazepines regularly, you need medical supervision to stop. It’s about protecting your life. Professional benzo withdrawal treatment provides the structured, gradual approach needed for a safe recovery.
Medical Approaches to Benzo Withdrawal Treatment
Given the dangers, benzo withdrawal treatment must be medically supervised. The approach combines careful tapering, supportive medications, and sometimes specialized interventions.

Medically-Supervised Tapering Strategies
Gradual dose reduction (tapering) is the gold standard of care. It gives your brain time to readjust safely. The two main approaches are:
- Direct Taper: Slowly reducing the dose of the benzodiazepine you are currently taking.
- Substitution Taper: Switching to a long-acting benzodiazepine like diazepam (Valium) before tapering. This is often preferred for those on short-acting or high-dose benzos, as Valium’s long half-life allows for a smoother reduction.
The Ashton Manual is a key resource providing evidence-based tapering schedules. However, any schedule must be individualized by a doctor based on your specific needs. Medication-Assisted Treatment (MAT) programs can offer expert guidance on this process.
Adjunctive Medications to Manage Symptoms
While tapering is the core treatment, other medications can help manage withdrawal symptoms:
- Anticonvulsants (e.g., carbamazepine) can reduce seizure risk and anxiety.
- Beta-blockers (e.g., propranolol) help with physical symptoms like rapid heart rate and tremors.
- Non-benzo sleep aids (e.g., trazodone) may be used for short-term insomnia, though non-pharmacological approaches are often preferred.
These medications play a supportive role and do not replace the need for a gradual taper.
The Role of Flumazenil in Benzo Withdrawal Treatment
Flumazenil is a medication that can block or reverse the effects of benzodiazepines at the brain’s receptor level. When given in low, slow doses, it is thought to help reset these receptors, potentially speeding up the brain’s recovery. Research on flumazenil for dependence suggests it may reduce withdrawal intensity, shorten detox duration, and lower relapse rates. However, its use is specialized and requires experienced medical professionals, as rapid administration can trigger seizures.
When is Inpatient Benzo Withdrawal Treatment Necessary?
While many can taper as outpatients, an inpatient setting is safer for some. It is generally recommended for:
- High-dose dependence
- Polysubstance use (e.g., with alcohol or opioids), which complicates withdrawal. Inpatient Rehab for Drugs can manage multiple dependencies.
- A history of seizures during previous withdrawal attempts.
- Severe co-occurring psychiatric conditions.
- Lack of a stable, supportive home environment.
Inpatient programs provide 24/7 medical care and a controlled, trigger-free environment, which can be critical for a safe and successful withdrawal.
Comprehensive Recovery: Beyond Medical Detox
Medical detox is a critical first step, but it’s not the end of the journey. True recovery from benzodiazepine dependence involves addressing the whole person—mind, emotions, and lifestyle—to build a foundation for a life free from medication.

Acute vs. Protracted Withdrawal (PAWS)
After the acute phase (the initial, intense withdrawal period), some people experience Protracted Withdrawal Syndrome (PAWS). Affecting 10-25% of long-term users, PAWS involves symptoms that can last for months or years. It’s characterized by “windows and waves”—periods of feeling well followed by a return of symptoms like anxiety, brain fog, mood swings, and sleep issues. This is a normal part of the brain’s extended healing process, and understanding it is key to long-term success, which is a factor in Drug Rehab Success Rates.
Non-Pharmacological and Holistic Support Strategies
Long-term recovery relies on healthy coping mechanisms, not just medication. Exploring Holistic Drug Treatment can provide powerful tools for healing.
- Therapy: Cognitive Behavioral Therapy (CBT) helps you change negative thought patterns, while Dialectical Behavior Therapy (DBT) teaches skills for managing intense emotions and distress. These Therapy Options are invaluable for navigating PAWS.
- Mind-Body Practices: Mindfulness, meditation, yoga, and Tai Chi reduce anxiety and help you reconnect with your body in a positive way.
- Lifestyle Support: Good nutrition provides the fuel your brain needs to heal. Regular exercise is a powerful natural mood booster that reduces stress and improves sleep.
Long-Term Implications and Building a Sober Life
While withdrawal can have lasting effects, your brain can heal. Cognitive recovery is real, but it requires continued abstinence and healthy habits.
Preventing relapse means building a life you don’t want to escape from. This involves:
- Aftercare Planning: A solid plan for managing stress and triggers, including ongoing therapy and medical check-ins.
- Support Groups: Programs like Narcotics Anonymous or SMART Recovery offer connection with peers who understand your journey.
- Continued Therapy: Addressing the root causes of your anxiety or insomnia is crucial. Therapy provides tools to manage these issues without returning to medication.
Building a sober life is about growth and creating a life that feels good to live. With patience and support, you can learn to steer challenges and thrive.
Frequently Asked Questions about Benzo Withdrawal
Here are answers to some of the most common questions about benzo withdrawal treatment.
How long does benzo withdrawal last?
The acute phase of intense symptoms typically lasts 5 to 28 days. However, 10-25% of long-term users experience Protracted Withdrawal Syndrome (PAWS), where milder symptoms can come and go for months or even years. The duration depends on the specific benzo, dosage, duration of use, and individual health.
Can I detox from benzodiazepines at home?
No. Detoxing at home without medical supervision is extremely dangerous and potentially fatal. Unlike many other substances, benzo withdrawal can cause life-threatening complications like grand mal seizures (occurring in 20-30% of unsupervised withdrawals), psychosis, and delirium. A medically supervised taper is the only safe method.
What is the first step to getting help for benzo dependence?
The first step is to contact a qualified healthcare professional, such as a doctor, psychiatrist, or addiction specialist. They will assess your situation and create a safe, individualized tapering plan. Never attempt to stop or reduce your dose on your own, as even small changes can trigger dangerous symptoms. If you’re unsure where to start, resources like ONEDrugRehab.com can help you find specialized providers.
Conclusion
Educating yourself about benzo withdrawal treatment is a vital first step. The journey away from benzodiazepine dependence is challenging, but recovery is absolutely possible.
This guide has emphasized one critical message: you need professional guidance. Medically supervised tapering, adjunctive medications, and professional support are necessities for a safe withdrawal, not luxuries.
Medical detox is only the beginning. True, lasting recovery involves a holistic approach that addresses your mind, body, and spirit. Therapy, mindfulness, proper nutrition, exercise, and peer support are all crucial for rebuilding your life and addressing the root causes of your initial struggles.
You don’t have to face this alone. Resources like ONEDrugRehab.com can help you find the right path forward. Every recovery journey is unique, which is why individualized care is so important.
Take the courageous step to reach out for help. Your health, safety, and your future are worth it. Explore holistic treatment programs to find a path that supports your whole-person recovery and know that a clearer, more authentic life is achievable.




