Types of Addiction Treatment: 10 Powerful Ways to Lasting Recovery 2025
Why Understanding Your Treatment Options Matters
Types of addiction treatment range from medical detox and residential rehab to outpatient counseling and peer support groups. Here’s what you need to know:
Main Treatment Levels:
- Medical Detox – Safe withdrawal management (1-3 weeks)
- Inpatient/Residential – 24/7 care in a facility (30-90 days)
- Partial Hospitalization (PHP) – Day treatment while living at home (4-8 hours daily)
- Intensive Outpatient (IOP) – Structured therapy sessions (10-20 hours weekly)
- Standard Outpatient – Weekly counseling sessions (up to 9 hours weekly)
- Sober Living – Transitional housing with peer support
Core Treatment Approaches:
- Medication-Assisted Treatment (MAT) – FDA-approved medications plus counseling
- Behavioral Therapies – CBT, motivational interviewing, contingency management
- Peer Support Groups – 12-step programs, SMART Recovery
- Holistic Therapies – Yoga, art therapy, mindfulness, acupuncture
If you’re feeling overwhelmed by addiction treatment choices, you’re not alone. About 10% of people aged 12 or older in the U.S. have alcohol use disorder, making it the most common substance addiction. Yet research shows that more than 90% of people who need addiction treatment do not receive it.
The good news? Addiction is a treatable chronic condition. Just like diabetes or high blood pressure, it can be managed successfully with the right approach. As one expert puts it: “Addiction is a chronic brain disorder, not a failure of willpower.”
This guide breaks down every major treatment option in simple terms. We’ll help you understand which level of care might work best, what each treatment type involves, and how to access help. Whether you’re exploring options for yourself or a loved one, you’ll have the knowledge to make informed decisions about recovery.
Understanding Addiction: Definition, Signs, Causes & Diagnosis
Before diving into treatment options, it’s crucial to understand what addiction actually is. The American Society of Addiction Medicine defines addiction as a chronic brain disorder involving compulsive seeking and taking of substances or performing activities despite harmful consequences.
The “4 Cs” framework provides a clear way to recognize addiction:
- Craving – Intense urges to use
- Loss of Control – Inability to limit use
- Compulsion – Continued use despite problems
- Consequences – Negative impacts on life, health, relationships
Addiction affects the brain’s reward system, particularly dopamine pathways. When someone uses substances repeatedly, their brain adapts by producing less natural dopamine, making normal activities feel less rewarding. This creates a cycle where the person needs the substance just to feel normal.
There are two main categories of addiction:
- Substance addictions – Alcohol, opioids, stimulants, cannabis, nicotine
- Behavioral addictions – Currently, only gambling disorder is officially recognized in the DSM-5
The DSM-5 outlines 11 criteria for diagnosing substance use disorders, grouped into four domains:
- Impaired control
- Social impairment
- Risky use
- Pharmacological criteria (tolerance and withdrawal)
More than 50% of people with substance use disorders have also had mental health problems at some point in their lives. This co-occurrence, called dual diagnosis, requires integrated treatment approaches.
Scientific research on brain changes shows that addiction literally changes brain structure and function, particularly in areas responsible for decision-making, impulse control, and reward processing.
Recognizing the Symptoms
Early recognition of addiction symptoms can make a huge difference in treatment outcomes. Common signs include:
Physical symptoms:
- Tolerance (needing more to get the same effect)
- Withdrawal symptoms when stopping
- Neglecting personal hygiene or health
- Changes in sleep patterns or appetite
Behavioral symptoms:
- Loss of control over use
- Continued use despite problems
- Spending excessive time obtaining, using, or recovering from substances
- Giving up important activities
Psychological symptoms:
- Cravings or strong urges to use
- Mood swings or irritability
- Anxiety or depression
- Denial about the severity of the problem
It’s worth noting that some people maintain high functionality while struggling with addiction. These “functioning addicts” may excel at work or maintain relationships while privately battling substance use. This can make recognition more challenging but doesn’t make the addiction any less serious.
Why People Get Addicted
Addiction doesn’t discriminate – it can affect anyone regardless of age, background, or circumstances. However, certain factors increase risk:
Genetic factors account for about 40-60% of addiction risk. If you have family members with addiction, you’re at higher risk.
Environmental factors include:
- Trauma or abuse
- Chronic stress
- Peer pressure
- Easy access to substances
- Mental health disorders
Protective factors that reduce risk include:
- Strong family bonds
- Involvement in school or community activities
- Positive role models
- Academic success
- Strong coping skills
The brain’s reward system plays a central role. All addictive substances stimulate dopamine release in the brain’s reward pathways, creating pleasurable feelings. Over time, the brain adapts by reducing natural dopamine production, making it harder to feel good without the substance.
The Continuum of Care: Levels & Settings in Types of Addiction Treatment
Think of addiction treatment as a continuum rather than a one-size-fits-all approach. The American Society of Addiction Medicine (ASAM) has developed criteria to help determine the appropriate level of care based on:
- Severity of withdrawal potential
- Biomedical conditions and complications
- Emotional, behavioral, or cognitive conditions
- Readiness to change
- Relapse potential
- Recovery environment
Here’s how the levels break down:
Level 1 – Outpatient Services:
- Standard outpatient: Up to 9 hours per week
- Intensive outpatient (IOP): 10-20 hours per week
- Partial hospitalization (PHP): 20+ hours per week, 4-8 hours per day
Level 2 – Intensive Outpatient:
- Structured programming while living at home
- Evening and weekend options available
- Ideal for those with stable housing and strong support systems
Level 3 – Residential Services:
- 24-hour care in a non-medical setting
- Typically 30-90 days
- Structured environment with peer support
Level 4 – Medically Managed Intensive Inpatient:
- Hospital-based care with 24/7 medical monitoring
- For severe withdrawal or medical complications
- Usually the shortest duration but highest intensity
The beauty of this system is that people can move between levels as their needs change. Someone might start in residential care and step down to IOP, then to standard outpatient as they progress.
Choosing Between Types of Addiction Treatment: Inpatient vs Outpatient
The choice between inpatient and outpatient care depends on several factors:
Inpatient/Residential is often recommended when:
- Severe addiction with multiple failed attempts at sobriety
- Unsafe or unsupportive home environment
- Serious medical or psychiatric complications
- History of dangerous withdrawal symptoms
- Lack of stable housing or transportation
Outpatient treatment works well when:
- Mild to moderate addiction severity
- Strong support system at home
- Stable housing and employment
- Motivation to change
- No serious medical complications
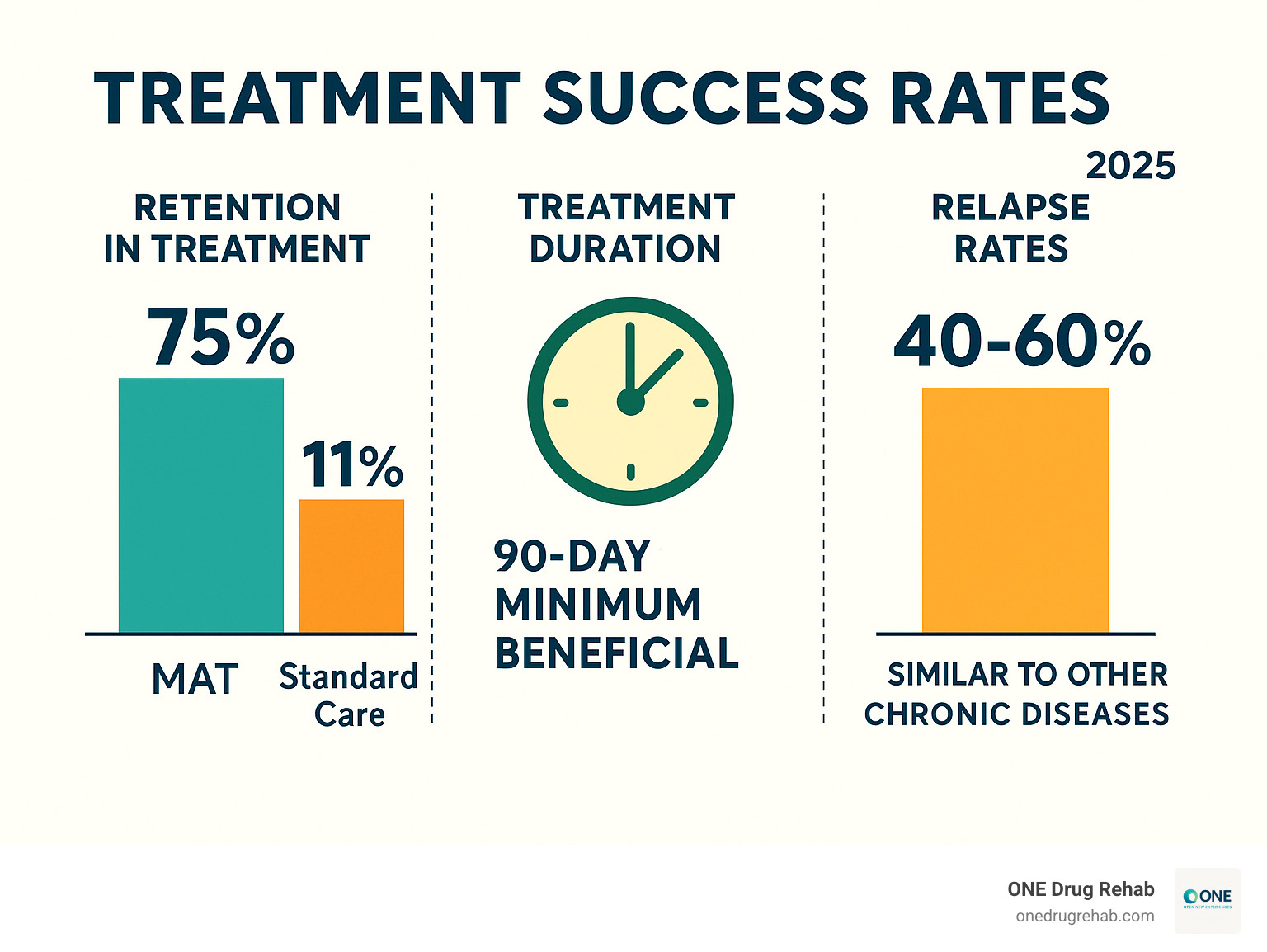
Research shows that individuals who stayed in treatment for 90 days or longer were more likely to remain abstinent compared to those with shorter stays. However, the setting matters less than the quality and duration of care.
Medical Detoxification: First Step to Safety
Detox is often the first step in addiction treatment, but it’s important to understand that detox alone is not treatment. It’s simply the process of safely managing withdrawal symptoms while substances leave the body.
Medical detox typically lasts 1-3 weeks and involves:
- 24/7 medical monitoring
- Medications to manage withdrawal symptoms
- Gradual tapering of substances when appropriate
- Preparation for ongoing treatment
Common withdrawal symptoms vary by substance but may include:
- Nausea and vomiting
- Sweating and tremors
- Anxiety and irritability
- Sleep disturbances
- Seizures (in severe cases)
For opioids, medications like buprenorphine or methadone can ease withdrawal. For alcohol, benzodiazepines may be used to prevent dangerous seizures. The goal is to keep people safe and comfortable while their bodies adjust.
Sober Living & Recovery Housing
Sober living homes provide a bridge between intensive treatment and independent living. These residences offer:
- Peer support and accountability
- Structured rules and expectations
- Drug and alcohol-free environment
- Continued access to treatment services
- Life skills development
Residents typically stay 3-12 months, though some remain longer. Rules often include:
- Maintaining sobriety
- Attending house meetings
- Completing chores
- Following curfews
- Participating in treatment or work
For young people, recovery high schools provide education in a sober environment. Recovery schools combine academic learning with addiction recovery support, helping students maintain sobriety while completing their education.
Core Treatment Modalities: Medication, Behavioral & Integrated Approaches
Effective addiction treatment typically combines multiple approaches custom to individual needs. The three main categories are:
- Medication-Assisted Treatment (MAT)
- Behavioral therapies
- Integrated care for co-occurring disorders
Research consistently shows that combining medication with behavioral therapy yields better outcomes than either approach alone. As one expert noted, “Medication should be the first line of treatment for opioid addiction, usually combined with some form of behavioral therapy or counseling.”
Medication-Assisted Treatment (MAT)
MAT combines FDA-approved medications with counseling and behavioral therapies. It’s considered the gold standard for treating opioid and alcohol use disorders.
For Opioid Use Disorder:
- Methadone – Long-acting opioid that prevents withdrawal and cravings
- Buprenorphine – Partial opioid agonist that reduces cravings with lower overdose risk
- Naltrexone – Blocks opioid effects, available as daily pill or monthly injection
For Alcohol Use Disorder:
- Naltrexone – Reduces alcohol cravings and blocks euphoric effects
- Acamprosate – Helps maintain abstinence by reducing withdrawal symptoms
- Disulfiram – Causes unpleasant reactions when alcohol is consumed
For Nicotine Addiction:
- Nicotine replacement therapy (patches, gum, lozenges)
- Bupropion (Zyban)
- Varenicline (Chantix)
MAT has been shown to:
- Increase patient survival rates
- Increase treatment retention rates
- Decrease criminal activity related to drug use
- Improve patients’ ability to gain and maintain employment
The whole-patient approach of MAT addresses not just the addiction but also medical, mental health, social, and vocational needs. This comprehensive care is what makes MAT so effective.
For those seeking MAT services, facilities like U Matter Detox Center offer specialized programs combining medication management with counseling support.
Evidence-Based Behavioral Therapies
Behavioral therapies help people change their attitudes and behaviors related to substance use. They’re essential for developing coping skills and preventing relapse.
Cognitive Behavioral Therapy (CBT):
- Helps identify and change negative thought patterns
- Teaches coping skills for handling triggers
- Often produces meaningful results in as few as 16 sessions
- Uses techniques like thought records and behavioral experiments
Motivational Interviewing (MI):
- Helps people find internal motivation to change
- Uses empathetic listening and collaborative approach
- Particularly effective for keeping patients engaged in treatment
- Based on four principles: express empathy, identify discrepancies, roll with resistance, support self-efficacy
- Provides tangible rewards for positive behaviors
- Often uses vouchers or prizes for drug-free urine tests
- Research shows 75% completion rates vs. 11% in standard care
- Particularly effective for stimulant addictions
The Matrix Model:
- Combines CBT, motivational interviewing, and 12-step facilitation
- Includes family involvement and relapse prevention
- Originally developed for methamphetamine addiction
- Provides structured 48-session framework
Dialectical Behavior Therapy (DBT):
- Focuses on emotional regulation and distress tolerance
- Particularly helpful for those with trauma histories
- Teaches mindfulness and interpersonal skills
- Effective for co-occurring mental health disorders
Integrated Care for Co-Occurring Disorders
Since more than 50% of people with substance use disorders also have mental health problems, integrated treatment is often necessary. This approach treats both conditions simultaneously rather than sequentially.
Common co-occurring disorders include:
- Depression and anxiety
- PTSD and trauma disorders
- Bipolar disorder
- Personality disorders
- ADHD
Integrated care involves:
- Coordinated treatment teams
- Psychiatric medications when appropriate
- Trauma-informed care approaches
- Specialized therapy techniques like EMDR (Eye Movement Desensitization and Reprocessing)
The key is recognizing that addiction and mental health disorders often fuel each other. Treating one without addressing the other typically leads to poorer outcomes and higher relapse rates.
Scientific research on effective treatment emphasizes that successful programs address the whole person, not just the addiction.
Complementary, Holistic & Peer Supports
While evidence-based treatments form the foundation of addiction care, complementary approaches can improve recovery by addressing physical, emotional, and spiritual needs.

Holistic therapies view addiction as affecting the whole person – body, mind, and spirit. These approaches can reduce stress, improve emotional regulation, and provide healthy outlets for expression.
Popular holistic therapies include:
- Yoga and meditation – Reduce stress and improve mind-body connection
- Art and music therapy – Provide creative expression and emotional processing
- Acupuncture – May help with cravings and anxiety
- Massage therapy – Reduces stress and promotes relaxation
- Equine therapy – Builds trust and emotional awareness through horse interaction
- Trip therapy – Uses outdoor activities to build confidence and teamwork
These therapies work best as complements to, not replacements for, evidence-based treatments. They can be particularly helpful for people who struggle with traditional talk therapy or need additional stress management tools.
12-Step & Peer Support Groups
Peer support groups provide ongoing community and accountability that many people find essential for long-term recovery. The most well-known are 12-step programs, but alternatives exist for those who prefer different approaches.
12-Step Programs:
- Alcoholics Anonymous (AA) for alcohol addiction
- Narcotics Anonymous (NA) for drug addiction
- Specific groups for different substances (Cocaine Anonymous, Marijuana Anonymous)
12-step programs offer:
- Free, widely available meetings
- Sponsorship relationships
- Structured approach to recovery
- Spiritual component (though not necessarily religious)
- Lifelong community support
Alternative peer support groups:
- SMART Recovery – Uses cognitive-behavioral techniques and self-management tools
- LifeRing – Focuses on personal responsibility and secular approach
- Women for Sobriety – Designed specifically for women’s needs
- Refuge Recovery – Buddhist-based approach to addiction recovery
Research shows that 12-step facilitation can improve clinical interventions but works best when combined with professional treatment rather than used alone.
Holistic Therapies in Recovery
Holistic approaches recognize that addiction affects every aspect of a person’s life. By addressing physical, emotional, and spiritual needs, these therapies can complement traditional treatment.
Benefits of holistic therapies:
- Stress reduction and relaxation
- Improved emotional regulation
- Creative expression and processing
- Physical health and wellness
- Spiritual growth and meaning-making
- Social connection and community
Popular holistic approaches:
- Mindfulness and meditation – Develop awareness and acceptance
- Yoga – Combine physical movement with mental focus
- Art therapy – Express emotions through creative activities
- Music therapy – Use sound and rhythm for healing
- Nutrition counseling – Repair physical health damaged by addiction
- Exercise programs – Improve mood and physical fitness
These therapies can be particularly valuable for people who have experienced trauma, struggle with mental health issues, or need help developing healthy coping strategies.
Harm Reduction Strategies
Harm reduction acknowledges that not everyone is ready or able to achieve complete abstinence immediately. Instead of viewing this as failure, harm reduction focuses on reducing the negative consequences of substance use.
Common harm reduction strategies:
- Needle exchange programs to prevent HIV and hepatitis
- Naloxone distribution to prevent overdose deaths
- Safe consumption sites with medical supervision
- Medication-assisted treatment as a bridge to recovery
- Education about safer use practices
While controversial, harm reduction has been shown to:
- Reduce overdose deaths
- Prevent infectious disease transmission
- Engage people who might otherwise avoid treatment
- Serve as a pathway to eventual abstinence-based treatment
Harm reduction doesn’t mean giving up on recovery – it means meeting people where they are and helping them take steps toward better health and safety.
For families affected by addiction, resources like Rehab for Families provide education and support for loved ones navigating the recovery process.
Staying the Course: Relapse Prevention, Aftercare & Accessing Help
Recovery doesn’t end when formal treatment concludes. In fact, relapse rates for addiction are similar to those for other chronic medical conditions like high blood pressure and asthma. This doesn’t mean treatment has failed – it means ongoing management is necessary.
Relapse prevention strategies include:
- Identifying personal triggers and high-risk situations
- Developing coping skills for stress and cravings
- Building a strong support network
- Maintaining regular therapy or counseling
- Participating in peer support groups
- Taking prescribed medications as directed
- Practicing self-care and stress management
Aftercare planning should begin during treatment and include:
- Ongoing therapy or counseling arrangements
- Medication management plans
- Peer support group connections
- Sober living arrangements if needed
- Vocational or educational goals
- Family therapy or support services
- Emergency contact information and crisis plans
Many treatment programs offer alumni services, including:
- Regular check-ins with counselors
- Alumni support groups
- Social activities and events
- Continued access to resources
- Refresher sessions or “booster” treatments

Digital resources are increasingly important for ongoing support:
- Telehealth counseling sessions
- Recovery apps for tracking progress
- Online support group meetings
- Educational resources and tools
- Crisis hotlines and text support
Matching Types of Addiction Treatment to Your Life Stage
Types of addiction treatment need to be custom to individual circumstances, including age and life stage.
Adolescent treatment considerations:
- Family involvement is crucial
- Educational needs must be addressed
- Peer influence plays a major role
- Development of identity and independence
- Higher likelihood of co-occurring mental health issues
Adult treatment considerations:
- Work and family responsibilities
- Financial concerns and insurance coverage
- Childcare needs during treatment
- Relationship and marriage issues
- Career and professional consequences
Older adult considerations:
- Medical complications and medication interactions
- Social isolation and loneliness
- Fixed incomes and insurance limitations
- Cognitive changes and memory issues
- Grief and loss issues
Specialized populations may need custom approaches:
- Pregnant women require specialized medical care
- LGBTQ+ individuals may need culturally competent providers
- Veterans may benefit from trauma-informed care
- Healthcare professionals face unique professional consequences
Funding & Insurance Options
The Affordable Care Act (ACA) requires most insurance plans to cover substance use disorder treatment as an essential health benefit. The Mental Health Parity and Addiction Equity Act requires equal coverage for mental health and substance use services.
Insurance coverage typically includes:
- Inpatient and outpatient treatment
- Medication-assisted treatment
- Counseling and therapy services
- Partial hospitalization programs
- Intensive outpatient programs
For those without insurance:
- Medicaid covers addiction treatment in most states
- State-funded treatment programs
- Sliding-scale fee programs
- Grants and scholarships
- Payment plans and financing options
For help navigating insurance and finding affordable options, resources like Find Rehab Without Insurance provide guidance on accessing care regardless of financial situation.
Cost ranges for different treatment types:
- Outpatient treatment: Around $10,000 per month
- Inpatient treatment: $20,000-$30,000 per month
- Luxury facilities: $1,000-$3,000 per day
- State-funded programs: Free or low-cost based on income
Digital & Community Resources
Technology is changing addiction treatment access and delivery:
Telehealth benefits:
- Increased access in rural areas
- Reduced transportation barriers
- Continued care during illness or quarantine
- Privacy and convenience
- Lower costs than in-person care
Recovery apps and digital tools:
- Sobriety tracking and milestone celebrations
- Craving management techniques
- Meditation and mindfulness exercises
- Connection to online support groups
- Educational resources and information
Community resources:
- Local health departments
- Community mental health centers
- Faith-based recovery programs
- Volunteer recovery organizations
- Peer support specialists
Frequently Asked Questions about Addiction Treatment Options
What is the most effective type of addiction treatment?
There’s no single “best” treatment – effectiveness depends on individual needs, circumstances, and the quality of care. However, research consistently shows that:
- Longer treatment duration (90+ days) produces better outcomes
- Combination approaches work better than single modalities
- Medication-assisted treatment is most effective for opioid addiction
- Integrated care is essential for co-occurring disorders
- Strong therapeutic relationships predict better outcomes
The most effective treatment is one that’s custom to your specific situation and includes multiple approaches working together.
How long does treatment usually last?
Treatment duration varies widely based on:
- Severity of addiction
- Type of substance
- Co-occurring disorders
- Support system strength
- Previous treatment history
Typical timeframes:
- Detox: 1-3 weeks
- Inpatient/residential: 30-90 days
- Intensive outpatient: 3-6 months
- Standard outpatient: 6-12 months or longer
- Medication-assisted treatment: Often years
Many people benefit from ongoing support for months or years after formal treatment ends. Recovery is a lifelong process, not a destination.
Does relapse mean that treatment has failed?
Absolutely not. Relapse rates for addiction (40-60%) are similar to those for other chronic diseases like diabetes, hypertension, and asthma. When someone with diabetes has a blood sugar spike, we don’t say their treatment failed – we adjust their medication or lifestyle plan.
The same applies to addiction. Relapse often signals the need to:
- Resume or intensify treatment
- Try different approaches
- Address underlying issues
- Strengthen support systems
- Adjust medications
Many people experience multiple episodes of treatment before achieving long-term recovery. Each episode can provide valuable learning and bring someone closer to sustained sobriety.
Conclusion & Next Steps
Navigating addiction treatment can feel overwhelming, but you don’t have to figure it out alone. The most important step is reaching out for help – whether that’s calling a treatment center, talking to your doctor, or attending a support group meeting.
Key takeaways:
- Addiction is a treatable chronic condition, not a moral failing
- Multiple types of addiction treatment exist to meet different needs
- Longer treatment duration generally produces better outcomes
- Combining approaches (medication, therapy, peer support) is most effective
- Recovery is a lifelong journey that requires ongoing support
Your next steps might include:
- Consulting with a healthcare provider about treatment options
- Researching treatment programs in your area
- Verifying insurance coverage for addiction services
- Attending a support group meeting
- Talking to family or friends about your concerns
Seeking help is a sign of strength, not weakness. Millions of people have walked this path before you and found recovery. With the right support and treatment approach, you can too.
For objective information about treatment facilities and programs, resources like Rehab Facility Reviews can help you make informed decisions. As an independent directory, we’re here to provide unbiased information to help you find the right path forward.
Recovery is possible. The journey may not be easy, but with the right support and treatment, you can reclaim your life and build a future free from addiction.




