Why Dual Diagnosis Rehab Programs Matter for Complete Recovery
Dual diagnosis rehab programs treat both mental health conditions and substance use disorders at the same time. If you’re struggling with depression and alcohol dependence, or anxiety and drug use, these programs offer integrated care that addresses both issues togethernot separately.
Key Features of Dual Diagnosis Rehab Programs:
- Integrated treatment – One team treats both your mental health and addiction simultaneously
- Medical detox – Safe withdrawal management with 24/7 medical supervision
- Evidence-based therapy – CBT, DBT, and other proven methods for co-occurring disorders
- Medication management – Psychiatric medications plus medication-assisted treatment when needed
- Multiple levels of care – Inpatient, outpatient, and aftercare options based on your needs
According to the Substance Abuse and Mental Health Services Administration (SAMHSA), 17 million adults faced both a substance use disorder and mental illness in 2020. Yet despite how common co-occurring disorders are, finding the right treatment can feel overwhelming.
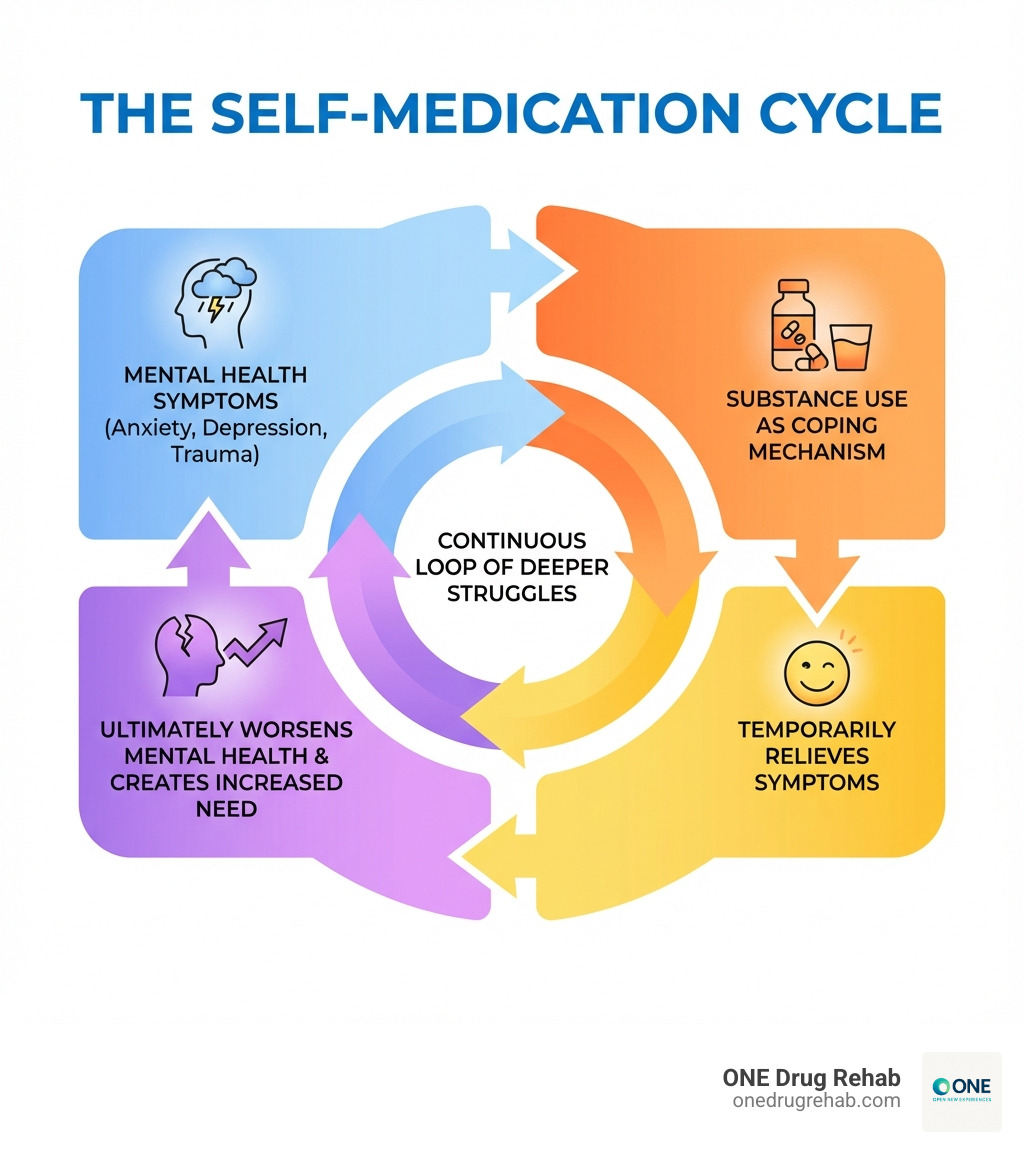
Mental health conditions and addiction often feed off each other. You might use substances to cope with anxiety or depressionwhat experts call self-medication. But substance use can also make mental health symptoms worse, creating a cycle that’s hard to break alone.
This guide explains what dual diagnosis treatment looks like, how to identify quality programs, and what to ask before committing to care. Whether you’re researching for yourself or someone you love, understanding your options is the first step toward integrated healing.
Understanding Dual Diagnosis: When Mental Health and Addiction Collide
Mental health and substance use disorders often go hand-in-hand. This section defines what a dual diagnosis means, how to recognize its signs, and the common conditions involved, helping you determine if a dual diagnosis rehab program is the right path for you or a loved one.
What is a Dual Diagnosis?
A dual diagnosis, also known as a co-occurring disorder, means a person has both a mental health condition and a substance use disorder (SUD). The focus is less on which came first and more on their complex relationship. Your mental health can influence substance use, and substance use can, in turn, affect your mental health.
Someone might self-medicate with alcohol to quiet anxiety. While this offers temporary relief, alcohol can worsen anxiety over time, creating a vicious cycle. Heavy substance use can also induce mental health symptoms. The key takeaway is that for lasting recovery, both conditions must be treated together, not in isolation.
To dive deeper into this topic, you can learn more about dual diagnosis from MedlinePlus. For specific treatment options, explore Dual Diagnosis Treatment on our site.
Recognizing the Signs and Symptoms
Identifying a dual diagnosis can be tricky as symptoms of mental health conditions and substance use disorders can overlap. However, knowing what to look for is an important step toward seeking help.
Here are some common signs of a mental health disorder:
- Mood swings: Dramatic shifts in mood, from extreme highs to deep lows.
- Social withdrawal: Pulling away from friends, family, and activities once enjoyed.
- Changes in sleep or appetite: Difficulty sleeping, sleeping too much, significant weight gain or loss.
- Loss of interest: No longer finding pleasure in hobbies or activities.
- Paranoia: Unfounded suspicion or distrust of others.
- Difficulty concentrating or making decisions.
- Feelings of hopelessness or worthlessness.
And here are some typical signs of a substance use disorder:
- Increased tolerance: Needing more of a substance to achieve the desired effect.
- Withdrawal symptoms: Experiencing physical or psychological discomfort when not using the substance.
- Neglecting responsibilities: Failing to meet obligations at work, school, or home due to substance use.
- Failed attempts to quit: Wanting to stop or cut down on substance use but being unable to.
- Risky behaviors: Engaging in dangerous activities while under the influence.
- Continued use despite negative consequences (for example, legal, health, or relationship problems).
- Spending a significant amount of time obtaining, using, or recovering from substance use.
If you recognize several of these signs in yourself or a loved one, it may be a signal that a dual diagnosis rehab program could be beneficial.
Common Co-Occurring Conditions
While the pairings of mental health conditions and substance use disorders vary, some combinations are more frequently observed. Understanding these common co-occurrences helps tailor treatment approaches.
Some examples include:
- Depression and alcohol use: As a depressant, alcohol may temporarily numb emotional pain but often worsens depressive symptoms long-term. Many with depression self-medicate with it to cope with sadness.
- Anxiety and benzodiazepine use: Benzodiazepines (like Xanax or Valium) prescribed for anxiety are highly addictive. People with anxiety may misuse these medications or other substances to calm their nerves, leading to dependency. For a holistic approach to anxiety, consider exploring Holistic Anxiety Treatment.
- PTSD and opioid use: Trauma survivors may use opioids for a temporary escape from intense emotional pain and flashbacks, which increases their risk of addiction.
- Bipolar disorder and polysubstance use: Individuals with bipolar disorder experience extreme mood swings. They might use stimulants during depressive episodes to boost energy or sedatives during manic episodes to calm down, leading to complex polysubstance use. The Mayo Clinic provides valuable Research on Bipolar Disorder and Alcoholism.
- Eating disorders and stimulant use: Stimulants (like amphetamines or cocaine) can suppress appetite, making them appealing to individuals with eating disorders who are trying to control their weight. This combination poses severe health risks.
For those dealing with depression, understanding all available avenues is crucial. Our guide on Holistic Depression Treatment offers additional insights. The National Institute on Drug Abuse (NIDA) also offers extensive research on co-occurring conditions, highlighting the scientific basis for integrated treatment.
Why Integrated Treatment is the Gold Standard for Recovery

For a long time, addiction and mental health were treated as separate issues, often by different specialists in different locations. This approach, while well-intentioned, often led to frustrating outcomes. Today, we understand that for individuals with a dual diagnosis, integrated care is the gold standard. This means treating both conditions simultaneously, in the same location, by the same team of professionals.
The Problem with Separate Treatment
Historically, people with co-occurring disorders faced the “wrong door” problemseeking help for their mental health only to be turned away because of their substance use, or vice versa.
When only one condition is treated, the untreated condition almost always sabotages recovery. For example, if someone with depression gets treatment for their alcohol use but their depression is not addressed, they are highly likely to relapse into drinking to cope with their untreated sadness. This increases the risk of relapse significantly. Despite the prevalence of co-occurring disorders, only 12.7% of people with these conditions actually receive treatment for both.
Benefits of an Integrated Approach
By addressing both the mental health condition and the substance use disorder at the same time, dual diagnosis rehab programs offer benefits that support more lasting healing.
These benefits can include:
- Higher success rates: Integrated treatment is associated with better long-term outcomes and more sustained sobriety.
- Improved quality of life: Many people report feeling better overall, with reduced symptoms of both conditions.
- Reduced relapse: Coping skills for both mental health and addiction triggers lower the likelihood of returning to substance use.
- More stability: Gains in mental health and sobriety can support more stable housing, employment, and relationships.
- Better physical health: Addressing both conditions holistically often improves overall physical well-being.
- A clearer path forward: Patients do not have to manage multiple systems or feel like they are being bounced between providers.
Understanding the full scope of what recovery can offer is empowering. You can explore the Benefits of Rehab and learn more about outcomes in our Drug Rehab Success Rate Guide.
To illustrate the advantages, consider this comparison:
| Feature | Sequential Treatment (Treating one issue, then the other) | Integrated Treatment (Treating both at once) |
|---|---|---|
| Relapse Rate | Higher, as untreated issues can trigger relapse | Often lower, due to comprehensive coping skills and symptom management |
| Treatment Engagement | Often sporadic; patients may drop out if one issue is not addressed | Typically higher, as patients feel understood and their full needs are met |
| Long-Term Outcomes | Less favorable; ongoing struggles with the untreated condition | More favorable; greater stability, improved well-being, and sustained recovery |
| Continuity of Care | Disjointed; requires navigating multiple systems | Cohesive; a unified team works on all aspects of healing |
| Patient Satisfaction | Lower, due to feeling fragmented or misunderstood | Higher, due to feeling holistically supported and cared for |
Navigating Your Options in Dual Diagnosis Rehab Programs
Finding the right dual diagnosis rehab program depends on your unique needs, the severity of your conditions, and your current support system. Below is a brief overview of common levels of care and therapeutic methods.
Levels of Care in Dual Diagnosis Rehab Programs
- Medical Detox: Often the first step when there is physical dependence on substances. Medical detox provides 24/7 supervision to manage withdrawal symptoms safely. A team of medical professionals focuses on comfort and safety. Learn more in Detox Treatment Options.
- Inpatient/Residential Rehab: For those needing a highly structured and supportive environment, inpatient rehab offers a live-in setting with intensive therapy, medical care, and support. This immersive environment removes many external triggers and allows deep focus on healing from both mental health issues and addiction. Find more about this option in Inpatient Rehab for Drugs.
- Outpatient Programs (Partial Hospitalization Programs – PHP & Intensive Outpatient Programs – IOP): These options provide flexibility for individuals with a stable home environment and support system.
- Partial Hospitalization Programs (PHP) usually involve several hours of programming on multiple days each week.
- Intensive Outpatient Programs (IOP) offer fewer hours per week but still provide structured therapy and support, allowing individuals to maintain some responsibilities like work or school.
Our Outpatient Rehab Programs Complete Guide provides an in-depth look at these options, and you can also compare them in How Do Residential and Outpatient Rehab Programs Compare.
Core Therapeutic Approaches
Effective dual diagnosis rehab programs rely on evidence-based therapies that address both mental health and addiction.
- Cognitive Behavioral Therapy (CBT): Helps individuals identify and change thought patterns and behaviors that contribute to substance use and mental health symptoms.
- Dialectical Behavior Therapy (DBT): Focuses on mindfulness, distress tolerance, emotion regulation, and interpersonal effectiveness. It is often used for people with intense emotional dysregulation.
- Eye Movement Desensitization and Reprocessing (EMDR): Frequently used for trauma-related issues, EMDR helps reprocess distressing memories and reduce their emotional impact.
- Group Therapy: Sharing experiences with peers facing similar challenges can be powerful. Group therapy reduces isolation and offers support. Learn more in What does Group Therapy help Addiction.
- Family Therapy: Addiction and mental illness affect the entire family. Family therapy improves communication, resolves conflicts, and educates loved ones on how to provide support.
- Holistic Therapies: Many programs add holistic approaches such as yoga, meditation, art therapy, music therapy, or equine therapy. These can support stress reduction and emotional expression. Explore more in our Holistic Treatment Programs guide.
The Role of Medication in Treatment
For many individuals in dual diagnosis rehab programs, medication is an important tool for stabilizing mental health symptoms, managing cravings, and supporting recovery. Medication is not a standalone solution but part of comprehensive care.
- Medication-Assisted Treatment (MAT): Uses FDA-approved medications, alongside counseling and behavioral therapies, to treat some substance use disorders. For opioid use disorder, medications like Buprenorphine and Naltrexone can reduce cravings and withdrawal symptoms, improve retention in treatment, and lower overdose risk.
- Antidepressants: Help regulate mood and can be crucial for treating depression and some anxiety disorders.
- Mood stabilizers: Used for conditions such as bipolar disorder, these medications help manage mood swings.
- Anti-anxiety medications: Sometimes used short-term for severe anxiety symptoms and prescribed with care due to their potential for dependence.
Effective medication management includes careful assessment, prescribing, monitoring, and adjustment by a psychiatrist or medical doctor so that medications remain safe, effective, and well integrated with therapy.
The Journey to Recovery: What to Expect
The path to recovery through dual diagnosis rehab programs is a process with distinct phases, from the initial assessment to long-term aftercare planning. It often involves loved ones and requires ongoing commitment.
Assessment, Duration, and Family Involvement
Your journey in a dual diagnosis rehab program typically begins with a thorough initial assessment. A team of professionalsincluding doctors, psychiatrists, therapists, and addiction specialistsevaluates the severity of both your mental health condition and your substance use disorder, along with your medical history, social support, and other needs. This assessment is the basis for an individualized treatment plan.
The duration of treatment can vary, often ranging from 30, 60, or 90+ days, depending on the intensity of the program and your progress. There is no single “right” length; the goal is to build a solid foundation for recovery.
Family involvement is often helpful. Many dual diagnosis rehab programs include family therapy sessions and educational programs for loved ones. These sessions can improve communication, support healthy boundaries, and help repair strained relationships.
Life After Rehab: Aftercare and Relapse Prevention
Completing an inpatient or intensive outpatient program is a major step, but ongoing support is important. Aftercare planning and relapse prevention strategies help you maintain gains made in treatment.
Aftercare plans are custom roadmaps designed to support continued sobriety and mental wellness. These might include:
- Continuing care: Stepping down from a higher level of care to a less intensive one, such as transitioning from PHP to IOP, or from IOP to weekly individual therapy.
- Sober living homes: Structured, supportive, and substance-free environments for individuals transitioning back into independent living. They offer accountability and a community of peers in recovery. Our Sober Living Homes Guide 2025 offers more information.
- Alumni programs: Many rehab facilities offer alumni networks, providing ongoing connection, support, and events for former clients.
- Ongoing individual therapy: Continued one-on-one sessions with a therapist reinforce coping skills and address new challenges.
- Support groups: Participation in 12-step programs (like AA or NA) or other recovery support groups (such as SMART Recovery, or Dual Diagnosis Anonymous) offers peer support and a sense of belonging. Find more options in our Recovery Support Groups resource.
Relapse prevention involves identifying triggers, developing coping strategies, and having a plan for challenging situations. It is about building resilience and knowing how to manage life’s ups and downs without returning to old patterns.
Unique Considerations for Different Populations
Many dual diagnosis rehab programs offer specialized tracks custom to the needs and experiences of different groups. These programs recognize that factors such as gender, age, and professional responsibilities can affect treatment engagement.
- Women’s programs: Often address concerns such as trauma, domestic violence, parenting challenges, and body image. For mothers, specifically, our Inpatient Rehab for Mothers Guide offers custom insights.
- Men’s programs: May focus on issues such as societal pressures, anger management, and emotional expression. More details can be found in our Inpatient Rehab Men Guide.
- Teen programs: Adolescents and young adults benefit from age-appropriate treatment that considers their developmental stage, family dynamics, and educational needs. Our Addiction Treatment Teens Complete Guide provides more information.
- Programs for professionals: High-achieving individuals such as doctors, lawyers, or executives often face unique pressures and concerns about confidentiality. Specialized programs for professionals address these issues while helping them protect their careers. Learn more in the Inpatient Rehab for Professionals Guide.
Finding and Affording the Right Dual Diagnosis Rehab Program
Starting the search for a dual diagnosis rehab program can feel overwhelming, especially when you are weighing quality and cost. Resources are available to help you steer this process and find a program that fits both your needs and your budget.
How to Find a Quality Dual Diagnosis Rehab Program
Not all programs are created equal. When researching dual diagnosis rehab programs, look for indicators of quality that suggest you will receive consistent, evidence-based care.
Consider the following:
- Accreditation: Look for facilities accredited by organizations like the Joint Commission (JCAHO) or the Commission on Accreditation of Rehabilitation Facilities (CARF). Accreditation signifies that a program meets established standards for quality and patient safety. Understanding Rehab Accreditation Standards can help you make informed choices.
- Staff Credentials: Check that the treatment team includes licensed and experienced professionals, such as psychiatrists, psychologists, licensed therapists (LCSW, LMFT, LPC), medical doctors, and addiction counselors.
- Evidence-Based Practices: Quality programs use therapies and treatments that research supports as effective for both mental health conditions and substance use disorders, such as CBT, DBT, and MAT.
- Individualized Care: Avoid programs that offer a one-size-fits-all approach. Treatment plans should reflect your specific dual diagnosis, personal history, and goals.
- Integrated Treatment Model: Confirm that the program truly integrates care for both conditions rather than treating them separately or in sequence.
- Aftercare Planning: Strong programs help you transition back into daily life with ongoing support and a clear aftercare plan.
A useful starting point for your search is the SAMHSA Treatment Locator, which lets you search for facilities by location and services offered, including those that treat co-occurring disorders.
Understanding Costs and Insurance Coverage
The cost of dual diagnosis rehab programs can be a concern for many people, but there are several ways to make treatment more affordable.
- Insurance Coverage: Under the Affordable Care Act (ACA) and the Mental Health Parity and Addiction Equity Act (MHPAEA), most health insurance plans cover mental health and substance use disorder treatment in a way that is comparable to coverage for medical and surgical care. Verify your benefits directly with your insurance provider to understand what your plan covers, including deductibles, co-pays, and out-of-network options. Our guide on Rehab Insurance Verification can walk you through the process.
- Medicaid: For individuals with limited income, Medicaid can cover a significant portion, or sometimes all, of the cost of addiction and mental health treatment. Many dual diagnosis rehab programs accept Medicaid. Find more information on Medicaid Approved Rehab Centers.
- Financing Options: Some facilities offer in-house financing plans, allowing you to pay for treatment in installments. There are also third-party healthcare lending companies that provide loans for treatment.
- State-Funded Programs: Many states offer publicly funded treatment options or grants for individuals who meet certain criteria.
- Sliding Scale Fees: Some non-profit organizations or smaller treatment centers offer services on a sliding scale, adjusting costs based on income.
The long-term costs of untreated dual diagnosisincluding health complications, legal issues, job loss, and strained relationshipsoften outweigh the investment in effective treatment. For an overview of typical expenses, refer to our Drug Rehab Cost guide, and if you are concerned about affording care, see Addiction Treatment Without Insurance.
Conclusion: Taking the First Step Towards Integrated Healing
You are more than a label. A dual diagnosis is not a life sentence but a starting point for a new, integrated path to wellness. It is a recognition that your struggles are complex, interconnected, and deserving of a comprehensive approach.
Treating both the mental health condition and the substance use disorder at the same time is often the most effective way to support lasting recovery. By seeking a dual diagnosis rehab program that addresses all of youmind, body, and spirityou are investing in a healthier, more stable future.
At ONEDrugRehab.com, we provide resources to help you compare your options and find the right fit, so you can access the integrated care you need.
Explore Co-Occurring Disorder Treatment options today.
Note: All references to programs, services, or resources now align with those offered or supported by ONE Drug Rehab, and do not promote competing services.




